Reshni's breastfeeding story
Monday 8 January 2018
Shared with permission from News Corp reporter Reshni Ratnam Courier Mail
Breast may be best when it comes to nourishing your newborn, but forcing this message on to new mothers is harmful.
Many mums are left feeling a failure as a parent because they can’t meet breast feeding demands, but this is so far from the truth.
As a mother of a premature baby, I’ve witnessed first-hand the difficulties some mums have producing enough milk to feed their babies — especially while these tiny humans are fighting to survive.
On November 3, my daughter Isla unexpectedly entered the world after just 29 weeks of gestation. She was tiny, weighing only 1240g.
I’d fallen over the afternoon before, leading to cramping, bleeding and a distressed baby. After hours under observation, my obstetrician broke the news to my very anxious husband and I — if our baby was to survive she would need to be delivered within the next 10 minutes.
We were about to have a baby — much earlier than expected — and were freaking the hell out.
Baby bottles were still on our list of things to buy. The steriliser my sister-in-law passed on was a foreign object to us and I hadn’t even considered buying a breast pump.
The first time I saw Isla in the critical care unit of Brisbane’s Mater Mothers’ Hospital will be a sight I’ll never forget. Tubes and monitors surrounded her pint-sized body which was nestled in a warm incubator.
I looked at her and thought “how can I take care of this baby?”
How would I feed her? Who was going to help me? Too many questions are asked, and more often than not, opinions are aired about why breast is best.
(Pic: Ric Frearson)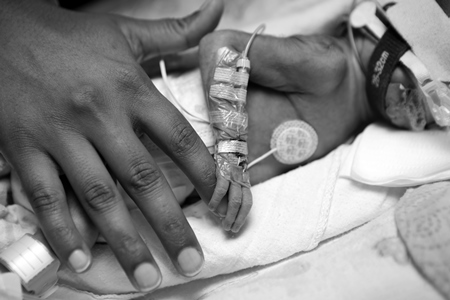
After spending every day since at the hospital, I’ve come to learn of other women’s emotional struggle.
With an oversupply of breast milk, I’m one of the lucky ones. I can’t imagine how much harder this would be if I wasn’t able to produce sufficient supply for Isla.
Stress and circumstances play a big role as to why many mums can’t breastfeed. And it’s time to stop and think about the hardship this can cause them. Some may have had a difficult pregnancy, while others are dealing with medical conditions, or bereavement.
Mater Mothers’ Hospital breastfeeding co-ordinator Julie Germain says mothers who are separated from their babies, who may be very sick, are at much greater risk of depression and anxiety.
“When they feel they can’t supply food for their baby it can be very emotional and traumatic,” she says.
We all laugh about it, but it really is “liquid gold”. My milk can help save the lives of sick babies.
Squeezing and syringing every drop of colostrum from my breasts, I was determined to help feed and nourish our baby.
The nurses couldn’t believe how much milk was being produced. I was hellbent on seeing my supply increase.
Some of my friends, who had “smooth births”, have told me they have never been able to produce milk for their babies.
And here I was after a fall, major surgery, and a premature baby, now able to produce milk just days after major surgery.
I have learnt that a mother’s generosity and oversupply of breastmilk can help restock the Queensland Milk Bank’s fridge and in turn save the lives of sick babies.
Donated breastmilk is in high demand in Queensland hospitals. And sadly, full term babies whose mums do not have a milk supply, are unable to access donated milk because there is such low stock for priority patients: premature bubs.
Access to the Queensland Milk Bank gives mums support at a crucial time while they can work on their supply.
Ms Germain says the milk bank comes in handy when mothers have missed out on the last few months of breast development in pregnancy to prepare for feeding.
“This, with separation and trauma and worry over a sick baby, can really challenge a mother and baby to successfully breastfeed,” she says.
Some bereaved mothers find it healing to donate their milk so it can help another baby survive.
The Queensland Milk Bank is run by the Royal Brisbane Women’s Hospital and is the largest public milk bank in the country, improving the outcome of more than 1400 premature babies.
Royal Brisbane and Women’s Hospital director of Neonatology Dr Pieter Koorts says using donor milk increases survival rates of almost 70 per cent, so the service is absolutely critical.
He says like the Blood Bank, they experience a lull in donations over the holiday period, and donations are essential to keep levels up during the festive season.
 As a first-time mum I have learnt that the initial few hours and days are very important to a feeding relationship after giving birth.
As a first-time mum I have learnt that the initial few hours and days are very important to a feeding relationship after giving birth.
However, many mothers of premature babies are separated during this time. Breastfeeding can be delayed and can affect milk supply.
For me, this is my way of saying thank you for looking after my baby and hopefully my donation will help other babies when they need it most.
All it takes is a simple questionnaire and a blood test before donated milk is accepted at the Milk Bank.
Contact the Queensland Milk Bank via Facebook, by phoning 3646 0542 or by sending an email to [email protected]